Dr. Barbara Bergin
Many of us have an exercise program we follow. We lift weights, do aerobics and/or attend a yoga class, and they consume large chunks of time in our day, and require planning to complete. Here are five simple exercises which require almost no extra time to complete, plus you can achieve important long-term benefits to
If it seems like I’m dissing women on the natural decrepitude of aging, first let me say the same things happen to
Whether you call them batwings, jiggly arms, or you remind yourself not to “wave like that,” our arms will eventually
I hope you’ve been reading Dr. Barbara Bergin’s humorous and informative series of blog posts about what happens to our
Not all patients come to see me for painful conditions. Some see me because they don’t like what they see
In a recent post, Brenda suggested if we wear tight leggings, some of us might want to cover our bums.
I have a girlfriend in Austin who always says I’m too dressed up for Austin. Sometimes she’s right and sometimes
“Do not do squats!” It’s almost a mantra for me, and I don’t know why. After all, squats, deep knee
Do you remember your mom scolding you when you reached across the table for the rolls before anyone else had
No, this isn’t a reference to a gunshot wound. First used in 1916, it’s a metaphor that refers to something
Many of my patients complain of pain in their knees when they stand up from a sitting position. It’s a
I often find myself telling my patients what not to do, instead of what TO DO. Frankly it’s easier to
If you’ve been reading my posts you know I often base my recommendations on the basis of how I earn
It’s that time of the year, and I’m already seeing the seasonal uptick in the number of ladder injuries. Interestingly,
Skiing, motorcycle, bicycle and horseback riding accidents remain a source of new patients for orthopedic surgeons. We see everything from
There are a lot of simple things we can do to prevent a fall. Many of the devastating injuries I
“I’m late! I’m late! For a very important date.” And just how important was that date, when you’re sitting in
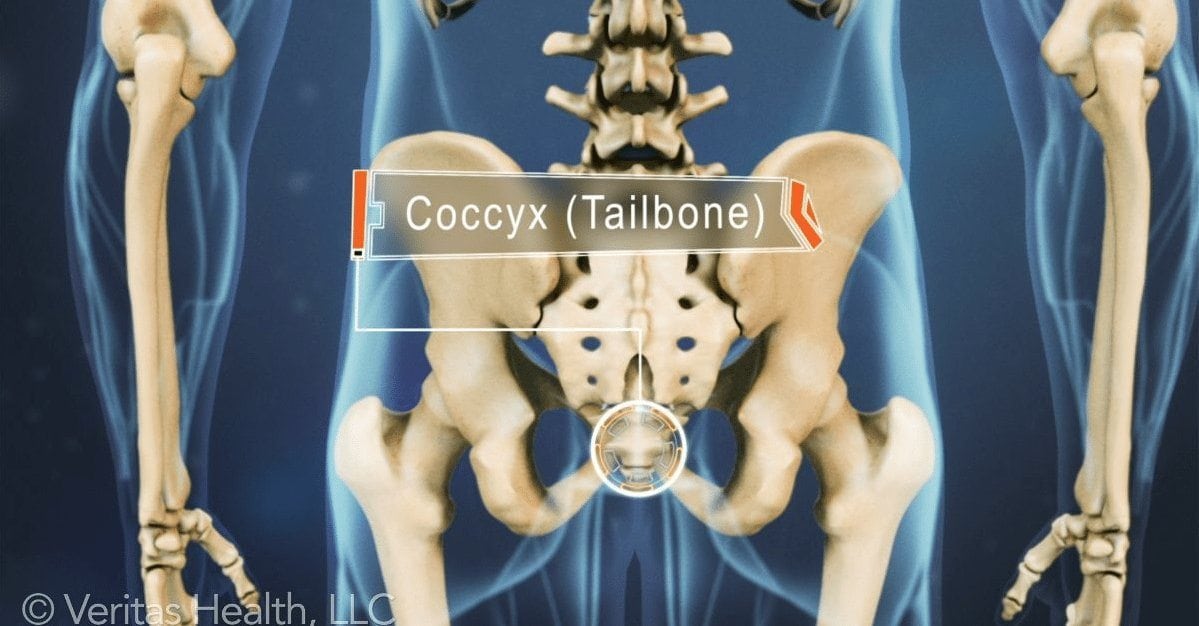
I have become the tail bone pain (coccydynia) expert of Central Texas. Recently I saw someone with coccydynia, from Waco,